Truly Understanding What Occurs on the Inside: My Journey with InsideTracker and GU Energy Labs11/27/2017 I’m not going to lie. I was a little bit skeptical getting my first blood draw from this company called Inside Tracker about 2 years ago. I had found them through a fellow trail and ultra-runner who had success with them. I agreed to a blood draw, but initially was only interested in them to track my Iron levels over time. I was a 23-year old seemingly healthy, ultra-marathon runner, who found increasing success and some notoriety in races ranging from 50 miles to 100km on technical mountain trails with challenging altitudes. All the while remaining relatively injury free. Having been a vegetarian for 4 years, I felt sure that I was eating well and staying well hydrated. My only “vice” was a moderate addiction to coffee and overall I thought I was consuming the right things to optimize my lifestyle. My delusion of a healthy body was about to be debunked. A simple blood biomarker analysis from a company called InsideTracker would punctuate what I felt was a lifestyle equilibrium and lead me on a journey culminating in an unfreezing of my former perceptions of nutrition, exercise, health and wellness, and lifestyle. Fast forward a year and a half and I am the fittest, healthiest, and happiest I have ever been. Sound like an exaggeration? Let me explain. Part 1: First things first; Inside-Who?? Founded by leading scientists, physicians, nutritionists and exercise physiologists from the likes of MIT, Harvard and Tufts University, InsideTracker is a blood-analytics company rooted in scientific research. They take your blood results and look at certain blood biomarkers and give recommendations on how to optimize them through supplementation, diet, and training modifications. Their goal is to help improve their client’s energy, metabolism, mood, sleep, performance, and recovery. On top of this, they are both passionate and knowledgeable about athletics and helping athletes understand their bodies. After reading more about them, I was excited to see what they had recommended for me. Part 2: “It’s all in your head. You’re a fit, healthy, young girl.” In general, as a fit endurance athlete, most general practitioners don’t take me too seriously when I say something feels off, and to their defense, I wouldn’t either. They’re are often over-worked, constantly surrounded by the sickest, most unhealthy individuals and have little time for guesswork. To them athletes are not life or death, chronically ill, or overweight individuals with high blood pressure. We need specialists in the field of athlete health, and for me finding specialists was the hardest part. In 2012, before I was taking this running thing seriously, I had record low iron levels and needed a transfusion. I decided against having it (I was naïve and wanted to go to Spain for my semester abroad) and ever since have been anemic. My Ferritin levels are rarely in the “normal” range. Ferritin levels are important because we need iron to make blood and transport oxygen to muscles for energy. I have tried a lot of things to get my ferritin to budge; new pills, liquids, or food forms. Despite all this, the number stays the same, staring back up at me, mocking me. My years of research experience in undergrad and beyond pushed me to continue to ask; “But, why??” “Why is it continually low, why do I not absorb the iron I am consuming?” No one I talked with ever investigated too deeply and eventually I assumed that every runner was as anemic as me and that was that. Add anemia to some uncontrollable race bonks, blurry vision, migraines around lunch, and chronic stomach pain and I was convinced that this was the life of an ultrarunner. Part 3: An initial look at the Inside, and it wasn’t pretty To say I was shocked from my blood results is an understatement. I thought I was a healthy individual who was in complete control of her body. How wrong I was. Getting these results made me take a realistic look at how I was nourishing, challenging and treating my body. The charade of arrogance about my own health was over. Transparency was scary. As I scanned the list of my results, I was stunned. My LDL was a bit too high. My Ferritin and Iron Group were too low. My Magnesium and Vitamin D were too low. My testosterone was too high and my cholesterol and glucose were on the high end of normal. InsideTracker not only communicates the results, but had already begun scientifically analyzing them and my current lifestyle and recommended changes. I got to work and started implementing some of their recommendations. InsideTracker knew that I’d had issues with anemia for years, so they recommended a different iron pill (ferrous sulfate) and instructed me to take it at night with vitamin C, far away from any other food consumption or workout. They also recommended I start taking Vitamin B12 to make sure that the anemia wasn’t caused by my inability to utilize this vitamin. This was the first I had even heard about this idea, but it made sense. 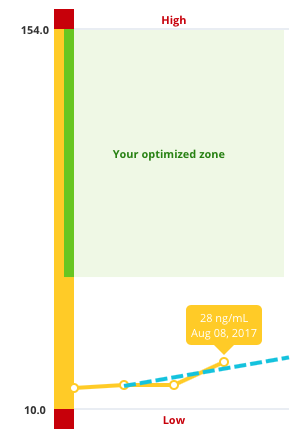 This helped a bit, but something still felt off. My follow-up test a couple of months later showed that my Vitamin D went up, Magnesium went slightly up, and my cholesterol went back to normal, however my glucose and ferritin stayed the same while my testosterone had tripled. As for the extreme elevation in testosterone, because it was extremely abnormal they suggested I go to a doctor. Part 4: “Google says you should have a beard, you don’t have one. I think you’re fine.” I went to a general care physician. I wish I hadn’t and wish that title was not quoting something he said. I’ll leave it at this. He thought everything was fine and sent me and my lack of facial hair on my way. Fast forward a week and I went where I should have in the first place. A doctor who specializes in women’s metabolic and hormonal disorders. She didn’t call me crazy and she didn’t laugh when I told her how I felt. She listened, chatted with me for an hour, and read through my InsideTracker results. She immediately ordered a follow-up blood test of markers not included on InsideTracker’s tests along with a scan of my ovaries. The next week after she had looked at my thyroid levels, FSH, LH, estrogen, and fasting insulin, she told me they were all way too low except the insulin, which was too high. She also told me my ovaries were covered in cysts. Part 5: “So I am pretty certain you have Polycystic Ovarian Syndrome.” Polycystic Ovary Syndrome (PCOS) is an endocrinpathy, where hyper-androgenism (high levels of androgen hormones like testosterone), chronic anovulation (missed periods), and polycystic ovaries are common.4 Say what?? In very basic level: What is PCOS? • It is a syndrome that is diagnosed by incorrect hormone levels in the body, missed periods, and cysts on the ovaries.3 It typically is a symptom of a larger disorder, Metabolic syndrome or Hypothyroidism, which have to do with incorrect regulation of endocrine hormones (5). What does it effect? • Blood Glucose: Insulin resistance is common and your body becomes less efficient at utilizing sugar due to an over production and desensitization to insulin. This disorder pre-disposes you to Type II Diabetes (2). • Hormone regulation: Certain hormone ratios are incorrect and this has cascade effects on other hormones in your body. This can affect things like being able to get pregnant (4). • Testosterone: Testosterone is high. This occurs because higher insulin levels can decrease the ability of proteins who clear these hormones out of your system (4). • A beard or male-patterned hair growth: Yes, you read that correctly. Apparently my Google-searching doctor wasn’t too far off, except this is not prevalent in all cases, but women with this disorder can exhibit male-patterned hair growth (4). • Thyroid: A decrease in the production of thyroid hormones that regulate appetite, metabolism, sleep, etc. This is 80% common in women with PCOS and it is either the leading cause of the other symptoms of PCOS, or it is a result of the hormonal imbalance (3). • Anemia: This one surprised me, but made sense! Hypothyroidism can cause anemia due to many factors dealing with things from the size of red blood cells, metabolic rate, and less absorption of iron through the gut (1) ! As my doctor explained to me the disorder, I had two thoughts resonating through my mind. “How am I going to manage this?” “I’m not crazy.” My doctor told me she thought I should tackle the low iron levels head on with an iron infusion. I declined politely. Then she said, it wouldn’t hurt to try and see if heme iron (animal-based iron) absorbs better in your body. I politely said no again, I had been vegetarian for 5 years, I was good. Then she prescribed me a low dose medication for diabetes/hypothyroidism, and some herbal based supplements to combat my stomach and hormone levels, I was sent on my way to report back in a month. Part 6: A Slice of Humble Pie I’d like to say that as soon as I started taking the supplements my doctor gave me, I felt like a new woman, but the adjustment wasn’t as easy as I thought it would be. It required more dedication on my end and at that time I only had 3 weeks of training left before the IAU Trail World Championships. I was not giving this disorder the respect it needed, but I thought I would be fine. The World Championships was a suffer fest. On top of spending the previous 10 days in Europe with minimal sleep, I missed a couple pills, ate mostly carbs in the small town of Bradia Prataglia and didn’t feel too great. I started the race carbo-loaded, which contrary to popular belief, was probably the worst thing I could have done, and suffered throughout the entire thing. I got home and immediately re-evaluated my priorities. I needed to take this disorder seriously if I wanted to run and recover well. I would never go into a race that unprepared again; some aspects of ultra-running we can control, and I controlled absolutely nothing. I called both InsideTracker and Roxanne, our GU energy labs nutritionist, to talk about ways to optimize my diet so my body could absorb nutrients and recover well. I kept a food diary for 2 weeks and was proud of it. Roxanne was not as proud, but she was extremely skilled at telling me that even though she could see I was trying, I was not eating the correct type or amount of calories necessary for someone with my condition and my intense training load. I wasn’t getting the nutrients I needed, even though I was eating enough calories; my body was still in a starved, undernourished state. I needed to increase my protein intake to 90-110 grams per day, decrease any empty carbohydrates (things like rice cakes, fruits, and cereals) that throw my blood sugar out of whack. I also needed to increase my consumption of healthy fats. Increasing fat, protein, and fiber would help keep my blood sugar stable. She also did not think my doctor’s recommendation to try meat was that outlandish since my disorder already made the absorption of nutrients more difficult. After some deep thinking on my diet, I finally threw in the metaphorical vegetarian hat. Part 7: I had a burger, won a race, got a CR, and my ferritin doubled within a month. I started eating meat and eliminating empty carbohydrate sources. 2 weeks later, I won and set a CR at the Mt. Hood 50 mile, and another 2 weeks later my ferritin was a whopping 28! That was more than double any number I had seen in over 5 years and I felt it! I started eating 90-100 grams of protein per day, upped my avocado game, and started packing snacks for races further from home. I have a weekly burger and some other sources of meat during the week. I’ve paid better attention to my body’s response to certain foods, and I have never felt as good in my entire life. Unless I slip up and eat incorrectly, my lunch-time blurry vision and headaches are gone. I finally wake up hungry in the morning and find myself with less stomach issues. My training and running has definitely improved and by switching to GU Energy Labs Peanut Butter or Chocolate Coconut Gels for racing, I have less crazy bonks. (Disclaimer: Those gels have fat in them!) Part 8: So, what exactly are you trying to say, Keely? 1. Trust your gut when something feels off. Athletes are a unique bunch and we know our bodies well. We are our biggest advocate because we don’t always have health care providers who know our bodies as well as we do. We don’t follow the “norm” of healthcare and neither should our expectations. We are all tough, but sometimes following up with something that feels off, no matter how big or small, is the smart thing to do. 2. Surround yourself by people who understand the athlete’s body. These people are great to have in your court. We all reach a point in our training where we plateau and are toeing that fine line of excellence. Having others around who understand your body and make recommendations can help take you to the next level. 3. Frequent blood testing is a good way to evaluate both your training and fitness loads, while realistically evaluating your health and eating habits. Get it done. It can help you with your performance, your life, and keep you more in tune with your body so that if something is out of whack, you can figure out what is behind it. 4. Eat what is right for you. Some diets resemble religion in the way they are preached. However, they are not a “one size fits all” and we need to eat what is best for our bodies, physiology, and mind. We need to be influenced by what is best for our own health and not influenced by outlandish diet crazes with claims you cannot rely on unrealistic or simply “trying” what seems to work for other athletes. Our bodies are our temples, you cannot trade it in for a new one. Be empowered to find out essential information that will help you manage and optimize your health. Because as much as running seems like life, the real race is not up the next mountain, but to have a long, healthy and happy life. Interested in seeing what’s on the inside? Check out InsideTracker’s website: www.insidetracker.com Sources: 1. Anemia in hypothyroidism. Antonijevic, et al. Medicinski Pregled. 01 Mar 1999. 52 (3-5): 136-140. http://europepmc.org/abstract/med/10518398 2. Insulin Resistance and the Polycystic Ovary Syndrome: Mechanism and Implications for Pathogenesis. Dunaif, Andrea. Endocrine Reviews, Volume 18, Issue 6, 1 December 1997, Pages 774–800. https://academic.oup.com/edrv/article-lookup/doi/10.1210/edrv.18.6.0318 3. PCOS and Thyroid Health. Tentrini, Dana. March 2014. http://hypothyroidmom.com/pcos-and-thyroid-health/ 4. Polycystic Ovary Syndrome (PCOS): Arguably the Most Common Endocrinopathy Is Associated with Significant Morbidity in Women. Enrico Carmina Rogerio A. Lobo The Journal of Clinical Endocrinology & Metabolism, Volume 84, Issue 6, 1 June 1999, Pages 1897–1899, https://doi.org/10.1210/jcem.84.6.5803 5. Polycystic Ovary Syndrom and Metabolic Syndrome. Gynekol, Ceska. 2015 Aug;80(4):279-89. < http://www.prolekare.cz/en/czech-gynaecology-article/polycystic-ovary-syndrome-and-metabolic-syndrome-52866> Happy Running Ya'll!!
0 Comments
Leave a Reply. |
Keely HenningerPortland, OR Archives
February 2021
Categories
All
|